Future of NY's Safety Net Providers in Hochul's Hands, Advocates Say
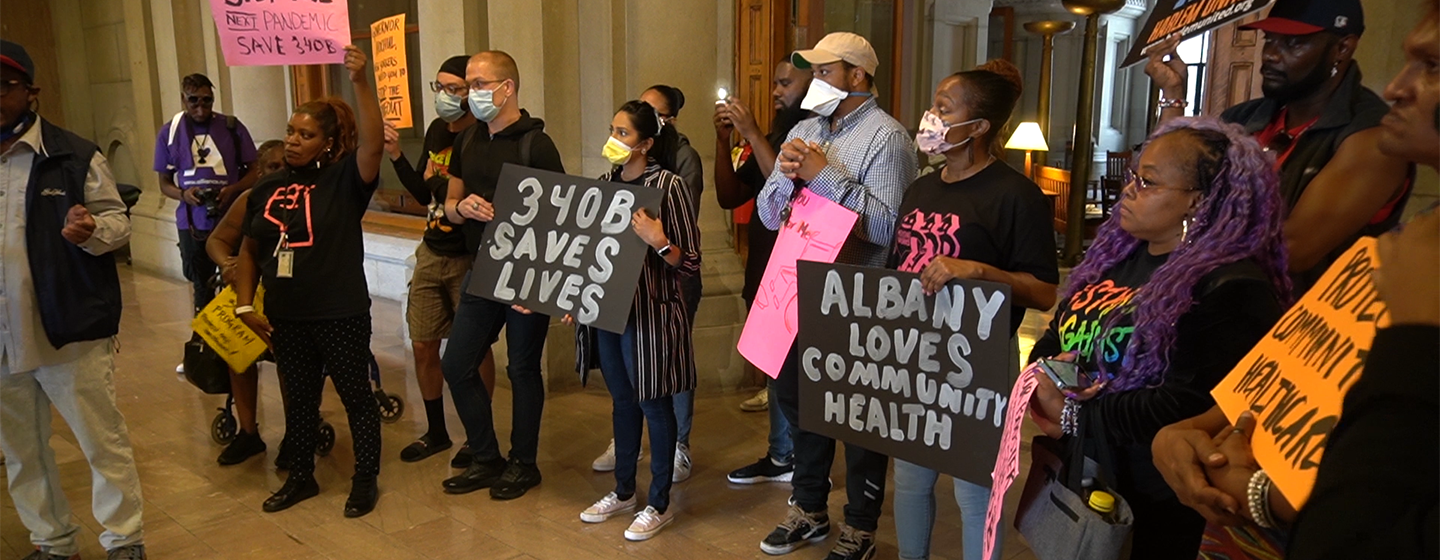
NY's Safety Net Providers and the Medicaid Pharmacy Carve-Out
Advocates are calling on Gov. Kathy Hochul to reverse a decision from the prior administration that could prevent certain safety net health care providers from taking advantage of a federal cost-savings program.
That program, called 340B, allows those providers to purchase prescription drugs at a discount and use those savings to provide services for underserved communities.
But a decision in 2020 from her predecessor, former Gov. Andrew Cuomo, could cut into that practice.
Cuomo had tasked a panel with finding areas in which the state could reduce spending for Medicaid, which makes up about a third of the state budget each year. The goal was to find $2.5 billion in cuts ahead of budget negotiations, which happen in March.
That panel, called the Medicaid Redesign Team II, ultimately hit that goal, recommending a series of ways the state could change how it funds the program.
Among them was a proposal to transfer what’s called the Medicaid pharmacy benefit from Medicaid managed care to a fee-for-service model. The panel had argued that could save the state at least $125 million the year after implementation.
Some analyses have challenged whether the proposal will actually save the state money, or be particularly effective at reining in costs.
Under the proposal, private plans that participate in Medicaid managed care would no longer process prescription drug claims on their own. Instead, the state Department of Health would take over those claims, and pay them directly.
Safety net providers have said that change would prevent them from continuing to receive savings from the federal 340B program. That means they would have less money to spend on services for underserved communities.
“I want our governor to think about, if this carve-out happens, you’re actually saying you don’t care about these individuals,” said Omari Edwards from the Albany Damien Center, one of the providers that anticipates cuts to services if the change goes through.
The change would take effect next April. It was initially supposed to be implemented the same year, but the Legislature negotiated a two-year delay in the 2020 state budget.
Because the Medicaid program is managed by the state, advocates have argued that Hochul could reverse the change unilaterally before it’s set to take effect. There’s also a bill in the Legislature, but it hasn’t moved.
A spokesperson for the state Department of Health defended the change, saying it would make the pharmacy reimbursement process more efficient, tighten up payment for those services, and be better for consumers.
"The 340B program is a Federal Program that is not being eliminated," said Jeffrey Hammond, the agency's spokesperson. "The Department is working with the impacted groups and is committed to ensuring a smoother transition."
Related

NY's HIV/AIDS Providers Want Hochul to Reverse this Cuomo-Era Change
The change could disproportionately impact organizations that offer medical services for people living with HIV/AIDS, those groups said in a letter to the Hochul administration Monday.


